Hemorrhoids, Anal Fissures and Rectal Prolapse- What’s the connection?
What can you do about them?
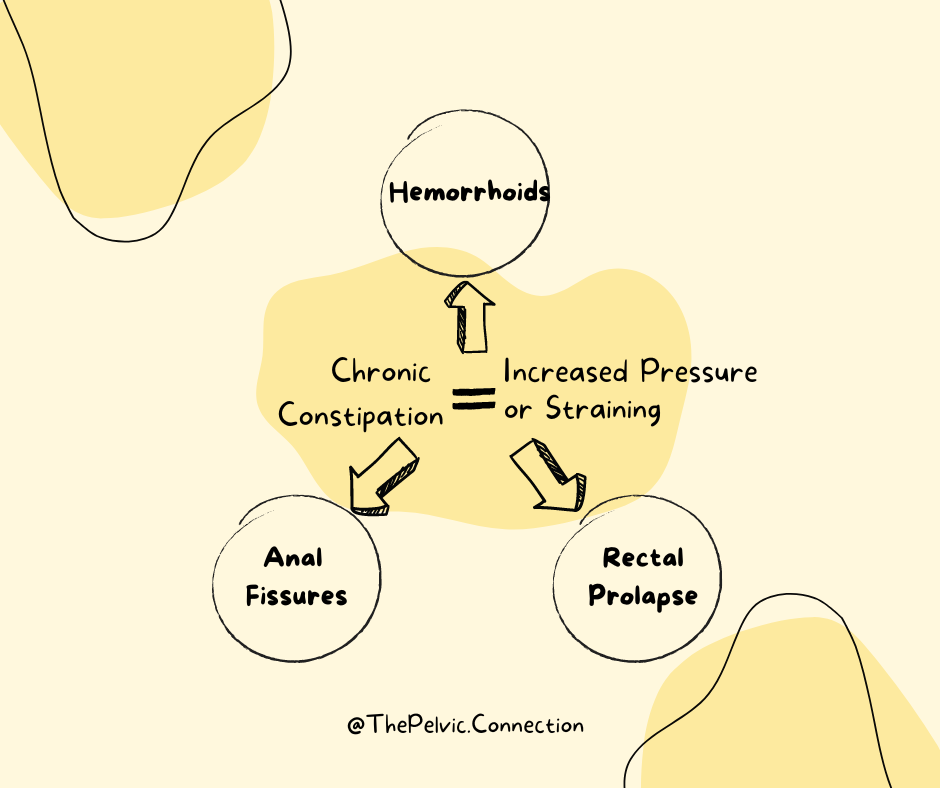
Have you ever wondered what’s common between hemorrhoids, anal fissures, and rectal prolapse? Yes, you are right, all these conditions affect the rectum and the anus, but there’s more to it than that!
Did you know that chronic constipation can cause all these issues if not addressed in a timely manner?
Chronic constipation brings along the problem of chronic straining, which increases the pressure on all the pelvic organs, blood vessels in the pelvic region, as well as the pelvic floor muscles.
This increase in pressure on the veins in the lower part of the rectum and the anus causes swelling and inflammation, which ultimately gives rise to hemorrhoids. Increase in pressure on these veins is also the reason hemorrhoids are so common during pregnancy.
The straining to force a bowel movement can also cause overactivity or tightness in the pelvic floor, as these muscles have to work harder to combat/offset the pressure coming from the top. This affects the pelvic floor muscles’ ability to effectively contract and relax, rendering them dysfunctional. This pelvic floor dysfunction is responsible for what is clinically referred to as outlet obstruction or puborectalis dyssynergia, which further perpetuates the vicious cycle
Trying to force a hard bowel movement through tight pelvic floor muscles can really stretch out the mucosal lining of the anal canal beyond its capacity, resulting in tearing, aka anal fissures.
Last but not least, chronic straining due to constipation can also cause rectal prolapse. Rectal prolapse is a downward displacement of the rectum in the anal canal or a forward protrusion towards the vaginal canal. Generally, this is triggered by reduced support to the rectum or the thinning of the wall between the V@gina & the rectum. The prevalence of constipation is as high as 67% in people with rectal prolapse.
Rectal prolapse can create two issues:
Pocketing of feces, and feeling of incomplete voiding— Reduced support of the rectum can affect its ability to push the feces out effectively. The protrusion of the rectum through the vaginal wall (Rectocele) creates a small pouch where the hard feces can get stuck leading to incomplete voiding.
Anal incontinence. This refers to the condition where the anus loses its ability to control the feces, resulting in leakage.
To avoid all these issues, Type 4 smooth sausage-like bowel movement is the most desirable! However, we have to be careful about the straining.
Treating the root cause is obviously the most important thing here! Constant straining increases the pressure on the pelvic organs, and creates tension in the pelvic floor muscles, ultimately causing pelvic floor dysfunction. The overactivity in the pelvic floor can make things worse, perpetuating the vicious cycle.
Along with the dietary changes & improving the hydration to address constipation, you should also:
Address the straining: Do not hold your breath and push with all your might. Instead, use the sound 'Moo’ for poo.
Use a squatty potty or a step stool to position your pelvic floor in a more relaxed state.
Address your hypertonic muscles through pelvic floor physiotherapy
Learn to manage pressure while lifting— again avoid straining and breath-holding. Try exhaling while lifting or use the cue “blow before you go!”
Engage in regular exercises to improve gut motility.
Hope this was helpful!
Xx
Mukta



What about hemorrhoids caused by pushing a baby out?? They just aren't going away. Thanks!